NEWS
Latest stories from the Gantik team.
18
Feb
2022
Single Use
Single-use devices
What does single-use mean?
Do not reuse. A single-use device is used on an individual patient during a single procedure and then discarded. It is not intended to be reprocessed and used again, even on the same patient.
Is single-patient use the same as single-use?
No. Single-patient use means the medical device may be used for more than one episode of use on one patient only; the device may undergo some form of reprocessing between each use.
Why shouldn’t they be reused?
The MHRA is aware of serious incidents relating to reuse of single-use devices.
Medicines and Healthcare products Regulatory Agency, an executive agency of the Department of Health
© Crown copyright, except single-use symbol..
Reuse can be unsafe because of risk of:
-
Cross-infection — inability to clean and decontaminate due to design.
- Endotoxin reaction — excessive bacterial breakdown products, which cannot be adequately removed by cleaning.
- Patient injury — device failure from reprocessing or reuse because of fatigue, material alteration and embrittlement.
-
Chemical burns or sensitisation — residues from chemical decontamination agents on materials that can absorb/ adsorb chemicals.
Also, if you reuse a single-use device you may be legally liable for the safe performance of the device.
Can I sterilize a single-use device?
Some single-use devices are marketed as non-sterile. These may require reprocessing, in line with the manufacturer’s instructions, to make them sterile and ready for use.
Check the manufacturer’s instructions for any limit on the number of times the unused device may be reprocessed. Once used on a patient, the device must be discarded.
Source: Click HERE
24
Sep
2021
Contamination Issues
“A study conducted by the University of North Carolina at Chapel Hill’s School of Dentistry Oral Microbiology Laboratory found that dental bib clips may be potential sources of cross-contamination in the dental office. As part of the study, researchers sampled 50 bib clips from hygiene and dental operatories. One out of five bib clips were found to have a presence of significant microorganisms. Of most concern were the pathogenic species found: pseudomonas, S. aureus and the enteric bacteria, E. coli. Bacteria from one patient can stay on the clip and be passed on to the next patient or dental healthcare worker. The species comprising the contamination on the clips were consistent with coming from saliva and/or dental plaque, skin or water lines. Ways to avoid the risk of bib chain contamination include effective sterilization of chains between patients or choosing a disposable bib holder that is discarded with the bib”
Click HERE for the article
16
Aug
2019
Bugs, Bibs and the chain of infection
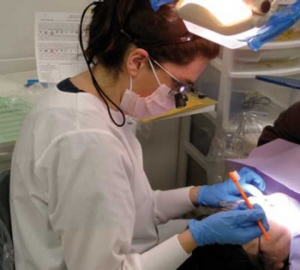
by Fiona M. Collins, BDS, MBA, MA 2011
Article and content from: RDH MAG
The goal of infection prevention protocols is to break the chain of infection. Five components are in this chain of infection, including the presence of a source/reservoir for pathogens that is also present at a level sufficient to cause disease. The source or reservoir can be you, a staff member, or a patient; or it can be an inanimate object.
Infection prevention protocols require the use of personal protection equipment that includes appropriate masks, nonsurgical or surgical gloves (procedure dependent), and the use of safety glasses. They also include the use of surface barriers and surface disinfectants that prevent and preclude indirect contact with pathogens.
Single-use, disposable products are recommended to help prevent the transmission of disease through indirect contact, and instruments must be appropriately processed and sterilized. By breaking the chain of infection, cross-contamination and disease transmission are prevented. One other type of “chain” that has recently come under scrutiny is the bib holder – not just the old-fashioned chain type of bib holder, but all reusable bib holders (chains, tubing, and clips).
A literal chain of infection?
While the bibs used in the dental office are single-use disposable items, the bib holders themselves typically are not. These may be the old-fashioned chain type composed of a series of tiny cylindrical metal balls with metal clips at the end, or more contemporary designs with stylized clips and smooth tubing. When you think about the location of bib holders against a patient’s skin and in close proximity to the source of contaminated spatter and aerosol generated during dental procedures, it is no surprise that pathogens can be found on bib holders.
Consider this: While a lower risk of cross-contamination and disease transmission may ensue from the use of reusable bib holders compared to many other items in the dental operatory, a risk of this occurring still exists, especially for the immune-compromised patient. Infection prevention protocols require that the chain of infection be broken and used bib holders are contaminated.
Bib chain studies
Let’s consider the outcomes of several small studies recently conducted on bib holders. One study, conducted by Noel Kelsch, RDHAP, assessed the role bib holders play in harboring microorganisms. In comparing levels of bacteria found on used bib holders with those found in airport restrooms, similar levels of bacteria were observed – as well as increased levels of microbial contamination in the crevices of the bib holders, including underneath smooth tubing. Of note, the bib holders sampled were reported to have already been disinfected with a hospital grade disinfectant.1
Kelsch’s findings are echoed in a study conducted by the University of North Carolina that led to the conclusion that bib holders are potential sources of contamination, with one in five bib clips sampled having significant levels of microorganisms. Importantly, bacterial growth on the bib holders was largely attributed to saliva and plaque as well as skin and flesh, and included E. coli and Staph aureus.2
Dr. John Molinari conducted a separate study on metal and coiled plastic bib holders. What were some of the findings? Bib holders tested after patient use without any cleaning or disinfecting had heavy bacterial loads, while treating bib holders with disinfectant wipes prior to testing greatly reduced but did not eliminate bacteria.3
The good news
The good news is that dental health-care personnel have become much more aware of bib holders as a source of microorganisms. In a new survey of dentists, dental hygienists and dental assistants, it was found that 82% were aware of bib holders as a potential risk for cross-contamination. When asked if this awareness had caused them to change their practice, 78% of those responding stated that it had.4 In offices that had changed their practice, bib holder treatments cited included heat sterilization, liquid chemical disinfection, and disinfectant wipes. The other option cited was the use of disposable bib holders.
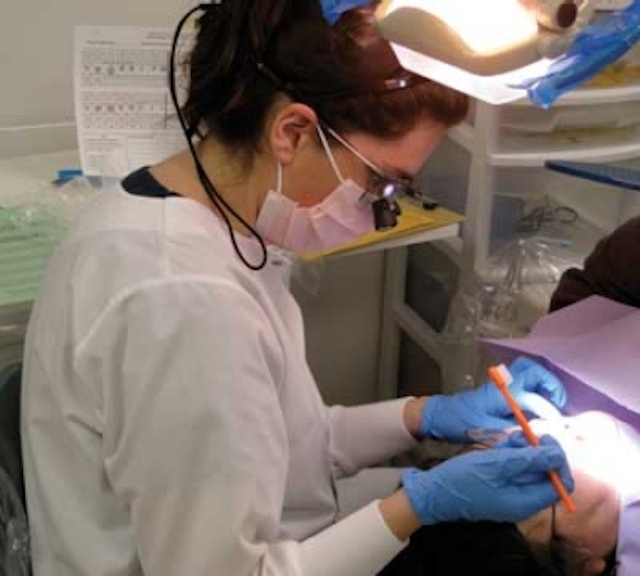 |
| Removing the reusable bib holder from the equation, and instead using single-use disposable bib holders, helps break the chain of infection in the dental office. |
Does it matter which bib holder is used, or how it is treated after patient use?
The answer is that it does. Logic suggests that the fewer crevices present on a bib holder and the smoother its surfaces, the fewer the inaccessible areas that can harbor microorganisms and the easier it is to clean and disinfect/sterilize the bib holder. Rubber tubing bib holders have smooth surfaces compared to, for example, chains, but in the case of hollow rubber tubing, the inner aspect of the tubing can be inaccessible for cleaning/disinfecting. In fact, in one of the cited studies, these were found to have a high level of contamination.
Stylized clips can also present challenges. What about treating reusable bib holders between patients? The use of surface wipe disinfectants on bib holders can reduce, but does not entirely eliminate, microorganisms present on bib holders – the disinfectant wipe cannot reach all crevices and inaccessible areas of the bib holder.
Beyond this, there are several other options to consider:
• Heat-sterilization (autoclaving) of bib holders is effective as long as all debris present was removed prior to autoclaving and the bib holder is autoclavable. Debris removal can be achieved using an ultrasonic bath.
• Immersion in a hospital grade disinfectant is also effective, again provided debris is first removed, and provided they are used appropriately and immersed for an appropriate length of time.
• Single-use, disposable bib holders
This third option — single-use, disposable bib holders — is an elegant solution. It costs no more than other options, saves time by removing the need to clean all debris from a bib holder and sterilize/disinfect it, and is the easiest and most effective solution. Most importantly, as with the single-use disposable bibs that are routinely used in the dental operatory, single-use disposable bib holders remove the possibility of cross-contamination.
Fiona M. Collins, BDS, MBA, MA, has authored and presented CE courses to dental professionals and students in the United States and internationally, and has been an active consultant in the dental industry for several years. Dr. Collins is a member of the American Dental Association and the Organization for Asepsis and Safety Procedures. Dr. Collins earned her dental degree from Glasgow University in Scotland and holds an MBA and MA from Boston University. She can be reached at fionacollins@comcast.net.
References
1. Kelsch N. Don’t clip that crud on me. RDH, 2011.
2. Oral microbiology lab, Chapel Hill School of Dentistry, University of North Carolina. Data on file.
3. Molinari JA. Microbial Contamination of Patient Napkin Holders. The Dental Advisor, June 2010.
4. Data on file.
28
Mar
2019
Gantik™ Presentation – Tissue World Milan 2019
Download our Tissue World Milan Presentation
27
Mar
2019
Tissue First – Press Release
“How a simple invention is about to change the tissue converting industry”
26
Mar
2019
Gantik™ Conference talk – Tissue World Milan 2019
Introduction to the World at Tissue World Milan 2019
10
Sep
2009
How did Gantik™ start?
Gail Shaw had a lightbulb moment when watching a boardroom struggling to tuck napkins and place napkins while having lunch. Gail thinks “why can’t they just stick?”
